State of the Nation 2026: progress in earlier diagnosis and the challenge of rising demand
In February 2026, the National Lung Cancer Audit (NLCA) published its latest State of the Nation report, which provides a picture of how lung cancer care is delivered across England and Wales. The report describes key aspects of care for people diagnosed in 2024 and shows encouraging progress in the number of people being diagnosed earlier, alongside growing pressure on treatment services across the pathway.
More people than ever before were diagnosed at an early stage of disease, largely driven by the continued expansion of the NHS Lung Cancer Screening Programme. This has led to a substantial increase in the number of patients eligible for, and receiving, treatment with curative intent. At the same time, the rising demand for thoracic surgery and systemic therapy services seems to have contributed to longer times between referral and starting treatment for some people.
This year’s findings highlight both how far lung cancer care has come and a need to ensure capacity keeps pace with progress.
Survival continues to improve Around 50% of people in England and Wales survived at least one year from the date of diagnosis, continuing gradual improvements seen in recent years.
Growth in rates of early diagnosis
In England, 40% of patients were diagnosed with stage 1 and 2 disease in 2024, which is an increase from 36% in 2023 and 32% in 2022. Wales has seen similar improvement, with 35% diagnosed at stage 1 and 2 in 2024, continuing the upward trend observed in recent years.
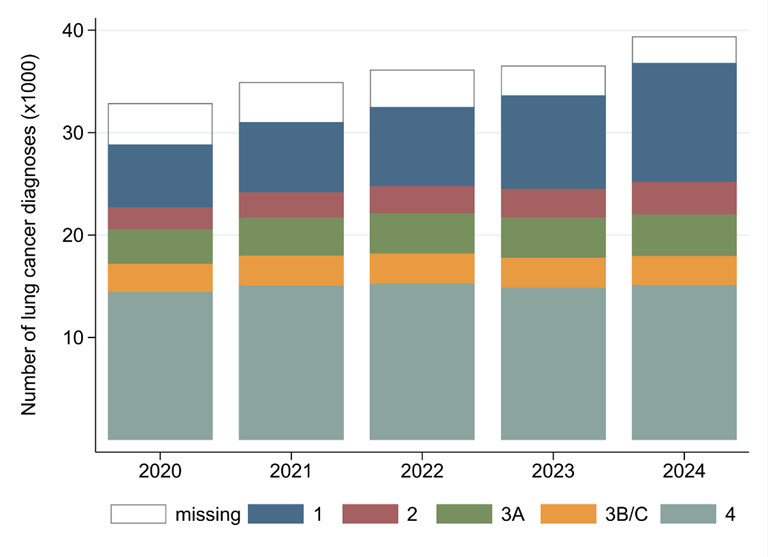
This represents a major success for lung cancer services and for patients, and the shift reflects the impact of the NHS Lung Cancer Screening Programme, which aims to identify cancers earlier when curative treatment is more likely to be possible.
More people receiving curative treatment, but services are under pressure
As more early-stage cancers are detected, the number of people receiving curative treatment has increased substantially. More than 8,900 patients received treatment with curative intent, representing an increase of over 60% since 2019. Surgery remains the principal mode of curative treatment, although radiotherapy can be preferable for some patients. In England, there were 7,878 people who had surgery to remove their lung cancer in 2024, compared with 6,547 in 2023.
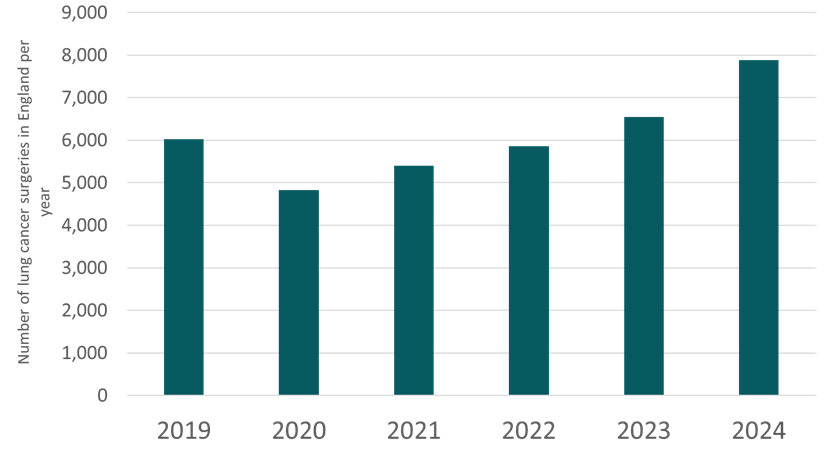
However, this growth in demand was placing an increasing strain on services.
Median waiting time from referral to surgery was 81 days in England and 91 days in Wales.
The report suggests that thoracic surgery capacity may be becoming misaligned with the rising demand. The report also found the median wait for radical radiotherapy was 98 days. The vast majority of patients exceeded national pathway targets for curative-intent treatment, and reducing unwarranted delays remains a priority.
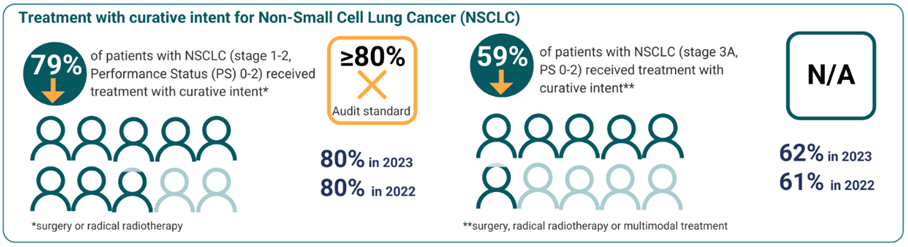
Another finding was that only around 60% of people with stage 3A non-small cell lung cancer and good performance status received curative treatment in 2024. Services are recommended to review their multidisciplinary team decision making and care pathways to identify and address barriers to potentially curative treatment, including the management of comorbidities and timely access to therapies.
Utilisation of systemic anti-cancer therapy remains below standards
Systemic anti-cancer therapy remains a cornerstone of treatment for locally advanced and metastatic lung cancer, yet uptake continues to fall below audit standards. Among people with stage 3B-C, stage 4 non-small cell lung cancer and good performance status, 63% received systemic therapy in England and 62% in Wales. Both remain below the national target of 70%, with substantial variation between regions.
Looking ahead
Earlier diagnosis is transforming lung cancer care, and we have seen a steady increase in survival rates. However, the full benefits of screening and modern therapies require the sustained monitoring of performance, along with targeted investment, to ensure the availability of surgery and oncological therapies meet patient demand. The NLCA will continue working with NHS organisations, Cancer Alliances and Health Boards to reduce variation, support quality improvement and improve outcomes for people with lung cancer across England and Wales.